How to recognize symptoms of Parkinson's disease early on
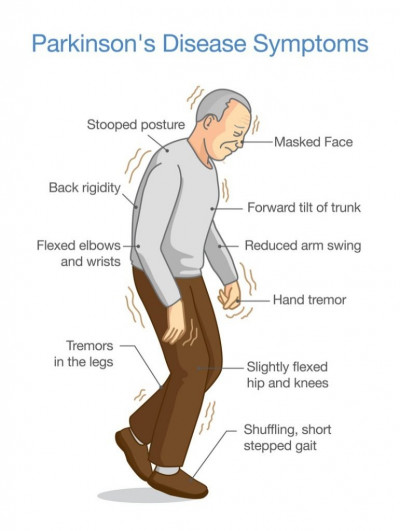
How to recognize symptoms of Parkinson's disease early on
Let me start off by a full disclosure, the last two and half years I spent as much time as I could with my dad, who sadly passed away after two weeks and a half of suffering. We held his funeral past Thursday June 15.
Late 2019, my dad was diagnosed with a Parkinson-related form of dementia called Lewy-body Dementia. I am not going to elaborate on the brain disease itself as there is already more than enough in-depth information written about this topic by people who are far more qualified than I am.
No this piece is about how you as family member, a son, daughter or partner might spot some early signs and what you perhaps can do or better what he or she could do to at least slow down the progress.
Early diagnosis is key and in case of my dad it was perhaps already too late to significantly have an impact in the development of his disease. Yet with all supplemental interventions we suggested and were able to persuade him to consider, we will never know effective they were.
Progression of his disease
In hindsight I am able to date when it might have started. Early March 2003 I purchased my first digital camera (a small point-and-shoot camera), which I purchased for my mom and dad to document moments in their daily life they spent with each other. That year turned out to be the last year they spent time together.
The first time my mom took a picture of my dad it surprised him in such a way, that the result was a bit awkward.
The way he looked and especially his facial expression was quite strange. At the time I didn’t think much of it. Even my dad, who saw the photo of himself was a bit shocked about how he looked, he never saw himself that up-close. This is a detail I never thought about, until recently after he passed away.
February 2004 just few days when my girlfriend and future wife Yvana had her life-saving surgery which would otherwise have left her paralyzed from the hip downwards, my mom was diagnosed with cervical cancer and passed away within days of the diagnosis.
Early 2015 my dad started complaining about muscle and bone aches, sometimes even pain upon which we went to several physicians ranging from an orthopaedic surgeon to those specialized in geriatric care.
In 2016 he would complain to me about his neighbor who would play music in the middle of the night. An investigation on my own did not conclusively give the answer whether this was true or not. It could have been my dad was mistaken where music came from.
Another strange phenomenon was how he thought to smell chlorine when he was in the kitchen.
A few months later in 2017, he decided to move places once more. What struck me most is how he was not walking as smoothly as he used to. Again, I did not pay enough attention to it, and assumed it was just a sign of aging.
Later that year, he talked about seeing things I could not observe nor dismiss myself. Things went from bad to worse. In 2018 it became really bad: not only did he have issues with his neighbor in his new apartment, but now he also talked about seeing my deceased grandmother with whom we all had an estranged relation. We shouldn’t speak ill of the dead, but she was a troubled person to say the least. For instance, my Indonesian grandmother would remind everyone who did not obey her orders, would be haunted by her after her death. After all, it was not uncommon for Indonesian people to believe forefathers would come and visit their offspring.
Weeks and even months after her death, my mother told me how she would see her mom visit her as an evil spirit. Almost 20 years later, my dad experienced the same.
This was either an apparition of my grandmother haunting him for real or a sign dad had started to hallucinate. I suspected the latter since he was once again complaining about a neighbor playing loud music late at night. However, all attempts to record this loud music were in vain.
In the meantime it became more obvious how his body became stiffer and he was moving in a more awkward way. Which made me suspect Parkinson’s disease and look up information on Parkinson's Disease. The literature didn’t just write about awkward movements but also described a tendency to hallucinate.
In 2019, after attempts to ban the devil (grandmom) from his body and his home proved to be in vain, dad tried to take his own life by overdosing on meds. Fortunately he was rushed to the hospital emergency room just in time. That same year, after thorough observation and clinical testing the doctors finally concluded that his disease, was indeed related to Parkinson’s disease.
After several months in the geriatric section of a mental hospital, he was finally able to return home with a slew of special meds dedicated to treat symptoms of Parkinson’s disease.
Only to be taken to hospital once more when he accidentally spilled boiling hot water on himself. After this event, it was clear he was unable to live by himself and he was admitted to a nursing home, where lived until the day he died on June 8.
I would visit him here at least twice a week, only to see him lose the battle with Parkinson’s. The medication he was prescribed did not catch on and sometimes he just refused to take them, since the meds made him feel drowsy , so he would sleep large parts of the day. Knowing he had little time left, he wanted to make the most of it.
For a long time I had already wanted to write about the onset of Parkinson’s disease, but procrastinated for various trivial reasons. At any rate, the suffering for my dad is over, may he rest in peace. He is in God’s hands now.
In case you are curious how this type of Parkinson's dease develops, here's more information on Lewy Body Dementia (LBD)
Dementia with Lewy Bodies
Dementia with Lewy Bodies is a type of progressive dementia that leads to a decline in thinking, reasoning and independent function. Its features may include spontaneous changes in attention and alertness, recurrent visual hallucinations, REM sleep behavior disorder, and slow movement, tremors or rigidity.Dementia with Lewy bodies is one of the causes of dementia, alongside other types of dementia like Alzheimer's disease and vascular dementia. "Lewy body dementia" (LBD) is a broad term that includes both dementia with Lewy bodies and Parkinson’s disease dementia. Here, we focus on the specific brain disorder called "dementia with Lewy bodies" (DLB).
The hallmark brain abnormalities linked to DLB are named after Frederich H. Lewy, M.D., the neurologist who discovered them while working in Dr. Alois Alzheimer's laboratory during the early 1900s.
Alpha-synuclein protein, the chief component of Lewy bodies, is found widely in the brain, but its normal function isn't yet known.
Lewy bodies may also be found in other types of dementia, including Alzheimer's disease dementia, and are a primary brain abnormality in Parkinson's disease dementia. Many people with Parkinson's eventually develop problems with thinking and reasoning, and many people with DLB experience movement symptoms like hunched posture, rigid muscles, a shuffling walk and trouble initiating movement.
This overlap in symptoms and other evidence suggest that dementia with Lewy bodies, Parkinson's disease, and Parkinson's disease dementia may be linked to the same underlying abnormalities in how the brain processes the protein alpha-synuclein. Many people with both DLB and Parkinson's dementia also have plaques and tangles — hallmark brain changes linked to Alzheimer's disease. When people have brain changes of more than one type of dementia, they are said to have mixed dementia.
Symptoms of dementia with Lewy bodies
Core symptoms of dementia with Lewy bodies include:- changes in thinking and reasonin
- fluctuating cognition that is delirium-like
- recurrent well-formed visual hallucinations
- REM sleep behavior disorder that involves acting out dreams
- spontaneous parkinsonism with slowness of movement, rest tremor, or rigidity.
Other symptoms may include:
- trouble interpreting visual information
- malfunctions of the "automatic" (autonomic) nervous system, which controls automatic functions of the body, such as sweating, blood pressure, heart rate, digestion and sexual response
- memory loss that may be significant, but less prominent than in Alzheimer's.
Diagnosis of dementia with Lewy bodies
As with other types of dementia, there is no single test that can conclusively diagnose dementia with Lewy bodies. Today, DLB is a "clinical" diagnosis, which means it represents a doctor's best professional judgment about the reason for a person's symptoms. The only way to conclusively diagnose DLB is through a postmortem autopsy.Most experts believe that dementia with Lewy bodies and Parkinson's disease dementia are two different expressions of the same underlying problems with brain processing of the protein alpha-synuclein. They recommend continuing to diagnose DLB and Parkinson's disease dementia as separate disorders.
The diagnosis is DLB when a person experiences dementia either before, at the same time as, or within one year of the onset of symptoms of Parkinson’s disease. In some cases of DLB, symptoms of Parkinson’s disease, like changes in movement, may never occur.
The diagnosis is Parkinson's disease dementia when a person experiences dementia at least one year (and usually several years) after the onset of symptoms of Parkinson’s disease. Parkinson's disease symptoms may include changes in movement like a tremor.
Since Lewy bodies usually coexist with Alzheimer's brain changes, it may sometimes be hard to distinguish DLB from Alzheimer's disease, especially in the early stages.
Key differences between Alzheimer's and dementia with Lewy bodies
Memory loss tends to be a more prominent symptom in early Alzheimer's than in early DLB. However, advanced DLB may cause memory problems in addition to its more typical effects on judgment, planning and visual perception.Movement symptoms are more likely to be an important cause of disability early in DLB than in Alzheimer's. However,
Alzheimer's can cause problems with walking, balance and getting around as it progresses to moderate and severe stages.
Hallucinations and misidentification of familiar people are significantly more frequent in early-stage DLB than in Alzheimer's.
REM sleep disorder is more common in early DLB than in Alzheimer's.
Disruption of the autonomic nervous system — such as causing a blood pressure drop on standing, dizziness, falls and urinary incontinence — is much more common in early DLB than in Alzheimer's.
Causes and risks
Researchers have not yet identified any specific causes of dementia with Lewy bodies. Most people diagnosed with DLB have no family history of the disorder, and no genes linked to DLB have been conclusively identified.Treatment and outcomes
There are no treatments that can slow or stop the brain cell damage caused by dementia with Lewy bodies. Current strategies focus on helping symptoms.If your treatment plan includes medications, it's important to work closely with your physician to identify the drugs that work best for you and the most effective doses. Treatment considerations involving medications include the following issues:
Cholinesterase inhibitor drugs are a common approach for addressing thinking changes in Alzheimer's. They also may help certain DLB symptoms.
Antipsychotic drugs should be used with extreme caution in Lewy body dementia, including both dementia with Lewy bodies and Parkinson's disease dementia. Although physicians sometimes prescribe these drugs for behavioral symptoms that can occur in Alzheimer's, they may cause serious side effects in as many as 50% of those with Lewy body dementia. Side effects may include sudden changes in consciousness, impaired swallowing, acute confusion, episodes of delusions or hallucinations, or appearance or worsening of Parkinson's symptoms.
Antidepressants may be used to treat depression, which is common with DLB, Parkinson's disease dementia and Alzheimer's. The most commonly used antidepressants are selective serotonin reuptake inhibitors (SSRIs).
Like other types of dementia that destroy brain cells, dementia with Lewy bodies gets worse over time and shortens lifespan.
Parkinson's Disease Dementia
Parkinson's disease dementia is a decline in thinking and reasoning skills that develops in some people living with Parkinson’s at least a year after diagnosis.About Parkinson's disease dementia
Parkinson’s disease dementia is a decline in thinking and reasoning skills that develops in some people living with Parkinson’s at least a year after diagnosis. The brain changes caused by Parkinson’s disease begin in a region that plays a key role in movement, leading to early symptoms that include tremors and shakiness, muscle stiffness, a shuffling step, stooped posture, difficulty initiating movement and lack of facial expression. As brain changes caused by Parkinson’s gradually spread, the person may also experience changes in mental functions, including memory and the ability to pay attention, make sound judgments and plan the steps needed to complete a task.The key brain changes linked to Parkinson’s disease and Parkinson’s disease dementia are abnormal microscopic deposits composed chiefly of alpha-synuclein, a protein found widely in the brain whose normal function is not fully understood. The deposits are called “Lewy bodies” after Frederick H. Lewy, M.D., the neurologist who discovered them while working in Dr. Alois Alzheimer’s laboratory during the early 1900s.
Lewy bodies are also found in other types of dementia, including dementia with Lewy bodies (DLB). Evidence suggests that DLB, Parkinson’s disease and Parkinson’s disease dementia may be linked to the same underlying abnormalities in the brain processing of alpha-synuclein. Another complicating factor is that many people with both Parkinson’s disease dementia and DLB also have plaques and tangles — hallmark brain changes linked to Alzheimer’s disease. When evidence of more than one type of dementia is found in the brain, it is called mixed dementia.
A study published on July 29, 2019 in Scientific Reports suggests that Lewy bodies are problematic because they pull alpha-synuclein protein out of the nucleus of brain cells. The study, which examined the cells of living mice and postmortem brain tissue in humans, reveals that these proteins perform a crucial function by repairing breaks that occur along the vast strands of DNA present in the nucleus of every cell of the body. Alpha-synuclein's role in DNA repair may be crucial in preventing cell death. This function may be lost in brain diseases such as Parkinson's and DLB, leading to the widespread death of neurons.
Prevalence
Parkinson’s disease is a fairly common neurological disorder in older adults, estimated to affect nearly 2% of those over age 65 and especially seems to affect people who work with pesticides.Causes and risk factors
Some studies have reported that the average time from onset of Parkinson’s to developing dementia is about 10 years. One large study found that about three-quarters of people who live with Parkinson's for more than 10 years will develop dementia. Before they develop dementia, they experience milder cognitive changes called mild cognitive impairment (MCI). Among individuals with normal cognition at Parkinson's diagnosis, about 30% will develop MCI after five years. However, cognitive changes and when they occur vary from person to person.Certain factors at the time of Parkinson’s diagnosis may increase future dementia risk, including advanced age, greater severity of motor symptoms and mild cognitive impairment.
Additional risk factors may include:
- the presence of hallucinations in a person who doesn’t yet have other dementia symptoms
- excessive daytime sleepiness
- a Parkinson’s symptom pattern known as postural instability and gait disturbance (PIGD), which includes “freezing” in mid-step, difficulty initiating movement, shuffling, problems with balancing and falling
Symptoms
Commonly reported symptoms include:- changes in memory, concentration and judgment
- trouble interpreting visual information
- muffled speech
- visual hallucinations
- delusions, especially paranoid ideas
- depression, irritability and anxiety
- sleep disturbances, including excessive daytime drowsiness and rapid eye movement (REM) sleep disorder.
Diagnosis
There is no single test — or combination of tests — that conclusively determines that a person has Parkinson’s disease dementia.
Guidelines for diagnosing Parkinson’s disease dementia and DLB are:
The diagnosis is Parkinson’s disease dementia when a person experiences dementia at least one year (and usually several years) after the onset of symptoms of Parkinson’s disease. Parkinson's disease symptoms may include changes in movement like a tremor.
The diagnosis is DLB when a person experiences dementia either before, at the same time as, or within one year of the onset of symptoms of Parkinson’s disease. In some cases of DLB, symptoms of Parkinson’s disease, like changes in movement, may never occur.
Outcomes
Because Parkinson’s disease and Parkinson’s disease dementia damage and destroy brain cells, both disorders worsen over time. Their speed of progression can vary widely.Treatment
There are no treatments to slow or stop the brain cell damage caused by Parkinson’s disease dementia. Current strategies focus on improving symptoms. If your treatment plan includes medications, it’s important to work closely with your physician to identify the drugs that work best for you and the most effective doses.Cholinesterase inhibitors — drugs that are the current mainstay for treating cognitive changes in Alzheimer’s — may help Parkinson’s disease dementia symptoms, including visual hallucinations, sleep disturbances and changes in thinking and behavior.
Carbidopa-levodopa — may be prescribed to treat Parkinson's movement symptoms. However, it can sometimes aggravate hallucinations and confusion in those with Parkinson's dementia or DLB.
Deep brain stimulation — deep brain stimulation (DBS) is currently contraindicated for Parkinson’s disease dementia (PDD). Although one small clinical study suggested it was safe for those with PDD, additional studies must be conducted to confirm its effectiveness.
Selective serotonin reuptake inhibitors (SSRIs) — used to treat depression, which is common in both DLB and Parkinson’s disease dementia.
Clonazepam and melatonin — may be used to treat REM disorder.
Caution: Antipsychotics that are used to treat behavioral symptoms should be avoided. About 60 percent of people with DLB who receive antipsychotic drugs experience worsening of Parkinson's symptoms, sedation, impaired swallowing or neuroleptic malignant syndrome (NMS). NMS is a life-threatening condition characterized by fever, generalized rigidity and muscle breakdown.
Conclusion
What you should take away from this story is how there are subtle and less subtle signs of this disease, which we don’t always spot in time. If I had known more about Parkinson’s disease earlier, he might have had a better chance of delaying the decline or coping better with the severity of it.One such advanced therapy might have been stem cell therapy. Yet, we also have to realize life is not eternal, our love is. Without death, there is no life. Death is part of life.
So stay focused on how we spend our life with our loved ones.


