How common are spinal or foot abnormalities?
How common are spinal or foot abnormalities?
A friend of mine sighed a few days ago that she had to return another pair of sandals because they hurt too much to wear due to a raised edge. She was comforted and given advice on all sides, after which it turned out that she had already tried most brands, most of which unfortunately were almost equally unbearable. She turned out to have a bone deformity in her foot, just like me, which is medically called 'hallux valgus', which means that you are almost condemned to wear only sandals or gym shoes with a wide forefoot. She also had osteoarthritis in her foot, which really makes you a 'princess and the pea'.
I don't have that misfortune, in my case the osteoarthritis is in my hip, which often makes me sigh how glad I am that I travelled a lot when I was young, so that I can now be a 'homebody', since both standing and walking can be painful.
My sweetheart has another problem, he always has to do extra exercises for his back, because there is a slight kyphosis in his upper back (and consequently a lordosis in the lower back).
Now I always thought that he was an exception in that, but imagine my surprise when I read that bone abnormalities are almost the norm rather than the exception, at least almost no one would have a perfectly formed spine or bone structure.
In short, let's dive into the phenomenon of 'bone abnormalities' and see what variations there are with an emphasis on abnormalities in the spine and the hallux valgus.
How common are spinal abnormalities
Spinal abnormalities, such as scoliosis, kyphosis, and lordosis, are not uncommon and can occur for various reasons including congenital deformities, age-related degeneration, disease processes, or idiopathic causes.
Scoliosis, an abnormal side-to-side curvature of the spine, is the most common type of spinal abnormality.
It can be mild and not cause any symptoms, or it can be severe and lead to pain, physical deformity, and in some cases, organ damage.
However, most cases of scoliosis are mild and do not require treatment.
Kyphosis, an exaggerated backward curve of the upper back, and lordosis, an exaggerated forward curve of the lower back, are also common spinal abnormalities.
Kyphosis can result from age-related degeneration or compression of the spine, while lordosis can be triggered by obesity, excessive kyphosis, or spondylolisthesis.
Early detection of spinal deformities is important for successful diagnosis, treatment, and outcomes.
Diagnostic tests such as X-rays, EOS imaging, and MRI can help identify and measure the degree of spinal curvature.
Treatment options for spinal abnormalities include non-surgical methods like medications, physical therapy, and bracing, as well as surgical interventions for severe cases.
The goal of treatment is to relieve pain, prevent further progression of the curve, and improve the patient's quality of life.
In summary, spinal abnormalities are relatively common and can vary widely in severity and impact on daily life.
Early detection and appropriate treatment can help manage these conditions effectively.
Definition of spinal deformities
The spine consists of an elegant stack of vertebrae and disks, which appear straight from the front and curved from the side, to keep the body erect and the head level. An abnormal curve in your spine, such as scoliosis or kyphosis, is known as a spinal deformity. It can affect your spine's ability to do its job, leading to pain, neurological problems, and mobility challenges. Spinal deformities can occur for a wide range of reasons, including birth defects, aging and degeneration, to trauma.
When the spine becomes weak or deformed, the rest of the body reacts. Muscles strain, lungs pump harder, and simple functions (such as walking) become difficult.
What are spinal deformities?
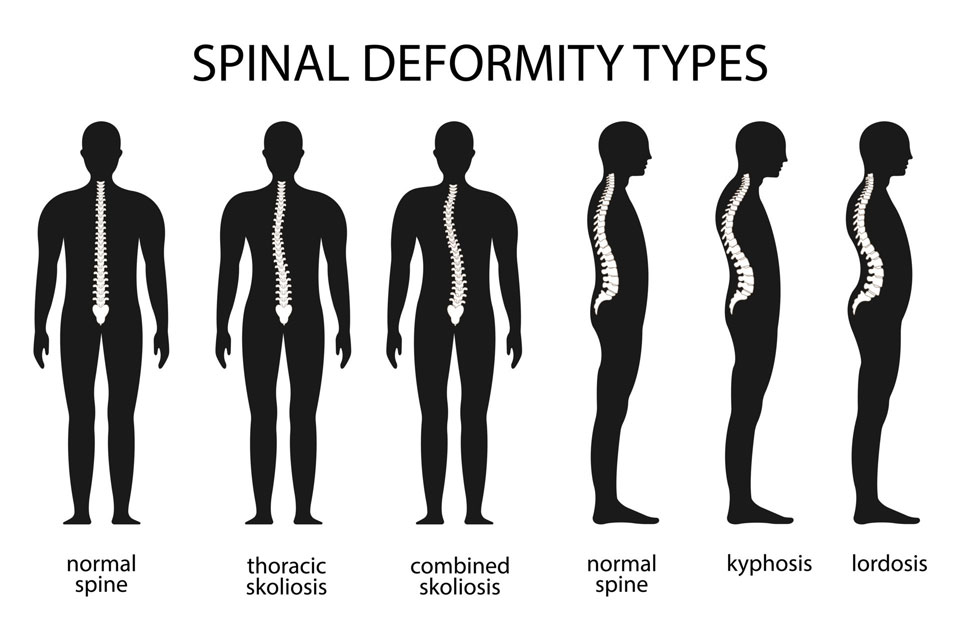
All spinal deformities involve problems of the curve or rotation of the spine. Common adult spinal deformities are scoliosis, kyphosis, and lordosis.
Kyphosis involves the upper back curving forward. The condition can create the form of a hump.
Lordosis is also known as swayback. This is a deformity of the lower back, in which it curves inward instead of outward.
Scoliosis is a frontal deformity in which the spine, when viewed straight on, curves to the left or the right. This curving ordinarily ends at the same time the skeleton stops growing but in adulthood, the curve can still progress slightly, often as a result of disk degeneration.
What are the symptoms of spinal deformity?
Symptoms differ, depending on the type of deformity. They may take the form of:
Pain. For scoliosis, this pain may occur in the upper spine and the ribs.
Feeling of being off balance or difficulty walking or standing. When the spine isn’t in correct alignment, the body and head aren’t either.
Visible curve (hunched over). In kyphosis, in particular, the outer curve in the upper back may be noticeable. In scoliosis, one shoulder blade, or hip, may appear higher than the other.
No symptoms. For some patients with mild deformities, the curves may not cause any symptoms.
When these spinal deformities lead to pain or affect your ability to perform daily activities, or if they cause dysfunction of the spinal cord/nerve roots, treatment (surgical and/or non-surgical) may be required.
How are spinal deformities diagnosed?
To diagnose a spinal deformity, a specialist will perform a physical examination and order x-rays of the spine. During an exam, the doctor will usually ask the patient to move into a few positions, such as a forward bend, in order to observe the spine as it moves. To see whether there is an underlying cause of the curve, magnetic resonance imaging (MRI) or computerized tomography (CT) scans may be recommended, in order to analyze the internal structure of the spine and surrounding area.
What are treatments for spinal deformities?
To treat spinal deformities, doctors look to relieve pain, lighten the strains on the spine, prevent deterioration of spinal structures such as disks and vertebrae, ease breathing if the lungs are affected, and reduce the appearance of the deformity.
When doctors determine the best approach, they consider whether a spinal deformity is stable or unstable.
Intervention may not be needed if the deformity is not progressing and the symptoms aren’t a problem for the patient. In these cases, specialists will monitor the curve and treat when necessary.
There are also several methods of physical therapies to treat spinal deformities by helping to reorient the spine and slow down the advancement of the curve.
When is spinal surgery necessary?
Surgery is performed is the curve is symptomatically compressing your organs or if the curve continues to progress or if the pain become severe and is unresponsive to medical and conservative care. Spinal surgery involves mobilizing and straightening the spine, and then placement of instrumentation with a spinal fusion in order to hold the spine in the new position and prevent further progression of the curve.
Neurosurgeons use a combination of screws and rods and bones (taken from another part of the body) to encourage growth of new bones in better positions.
Patients can expert to recover from this surgery within two months.
What are risk factors for spinal deformities?
Many cases of scoliosis have no identifiable cause. There are a few known genetic conditions that may put someone at risk of developing scoliosis, including cerebral palsy, muscular dystrophy, and achondroplasia, which is a condition affecting cartilage.
For kyphosis, risk factors include poor posture and fractures resulting from osteoporosis or injury.
Osteoporosis is also a risk factor for lordosis. Slipped vertebrae and obesity may also cause the condition.
Are spinal deformities treated differently in children, adults, and the elderly?
Children and adults are treated differently. When treating children with spinal deformities, nonsurgical treatments are often chosen since children's bones are still developing.
A brace, for example, can direct a child’s growing spine into the right alignment. In adults, the same treatment would be less effective because the spine is already rigid in its position.
In older adults, if osteoporosis is the underlying cause of the deformity, it may be treated with calcium, hormone replacement therapy, or weight-bearing exercises.
Bracing is another nonsurgical option for adults. It will not change the position of the spine, but it may ease pressure and pain. Orthotics (shoe inserts) can also help reduce back pain if the legs have been affected by the spine’s changing shape.
How normal are foot deformities like hallux valgus?
Hallux valgus, commonly known as a bunion, is one of the most common foot deformities, affecting a significant portion of the population.
It is characterized by the lateral deviation of the big toe and the medial deviation of the first metatarsal bone, leading to a bony bump at the base of the big toe.
The condition is more prevalent in women, with a ratio of 15:1 compared to men.
While the exact cause of hallux valgus is not fully understood, it is believed to be influenced by a combination of genetic factors, footwear, and foot mechanics.
Genetic predisposition plays a significant role, as more than 70% of people with bunions have a biological parent who has had them.
Additionally, wearing tight, narrow, or high-heeled shoes can exacerbate the condition or contribute to its development.
Hallux valgus can range in severity, with angles greater than 15° considered abnormal and angles of 45-50° considered severe.
The deformity is often progressive and can lead to pain, stiffness, and difficulty wearing certain types of shoes.
In summary, foot deformities like hallux valgus are quite common, particularly among women, and are influenced by a combination of genetic and environmental factors.
What is a bunion?
A bunion is a bony bump that forms at the base of your big toe. Bunions develop on the inside edge of your big toe joint — the metatarsophalangeal (MTP) joint. The MTP joint is where the base of your big toe meets your foot. The medical term for bunions is hallux valgus.
Visit a healthcare provider if you notice a bump on your big toe, especially if you’re experiencing pain, stiffness or numbness in your toes or feet.
Types of bunions
Bunions on your big toe from extra pressure are the most common, but they can form on other toes and for other reasons, too. Other types of bunions include:
Congenital bunions (congenital hallux valgus): Some babies are born with bunions.
Juvenile or adolescent hallux valgus: These are types of bunions that affect people younger than 18.
Tailor’s bunion (bunionettes): Tailor’s bunions form at the base of your little (pinky) toe. They’re usually the result of wearing shoes that don’t fit correctly or doing an activity that presses your little toe in toward your other toes.
How common are bunions?
Bunions are very common. Experts estimate that around one-third of the population have bunions.
What are the symptoms of a bunion?
The most obvious symptom of a bunion is the growth that forms at the base of your big toe. You can usually see and feel the bony bump. A bunion can cause other symptoms, including:
- pain or stiffness in your big toe.
- swelling.
- discoloration or redness.
- an inability to move or bend your big toe (you might feel pain or a burning feeling when you bend your toe).
- Difficulty wearing certain types of shoes, or pain that gets worse when you’re wearing shoes.
- corns or calluses (thickened skin).
- hammertoes (painful, tight toe tendons and joints).
- numbness in or around your big toe.
What causes bunions?
There’s not just one reason why bunions develop. It’s thought that a combination of factors — like family history, abnormal bone structure, increased motion and shoe choice — can cause them. When something puts extra pressure on your big toe joint for a long time (usually years), that pressure can push your joint out of its natural alignment and toward your other toes. Eventually, a bunion forms on your MTP joint when your body compensates for your toe being pushed out of its usual place.
The most common causes of extra pressure on your big toe joint include:
- wearing narrow or pointed shoes that crowd your toes (shoes with a narrow toe box)
- the way you walk (your foot mechanics)
- health conditions that cause inflammation (like rheumatoid arthritis or lupus)
- standing for a long time or working on your feet
Risk factors
Anyone can develop a bunion. Certain groups of people who are more likely to have bunions include:
- females
- people whose biological parents have bunions or issues with their foot mechanics. More than 70% of people with bunions have a biological parent who’s had them.
- People with a history of foot injuries (including athletes)
Complications of bunions
Having a bunion may increase your risk of:
- bursitis (painful, fluid-filled sacs around joints)
- hammertoes
- osteoarthritis
How are bunions diagnosed?
A healthcare provider will diagnose a bunion with a physical exam. They’ll examine your foot and ask about your symptoms. Tell your provider when you first noticed a bump near your big toe or if certain activities make your symptoms worse.
You might need to visit a podiatrist — a provider who specializes in caring for your feet.
What tests are done to diagnose bunions?
You may not need any tests for your provider to diagnose a bunion. Your provider will use foot X-rays to determine the overall alignment of your bones and your MTP joint.
How are bunions treated?
The most common bunion treatments include:
- Footwear changes: switching to shoes with wide, deep toe boxes can take pressure off your toes. You may be able to use a stretching device to widen shoes you already own.
- Bunion pads and taping: Over-the-counter (OTC) bunion pads cushion the area around a bunion to relieve pressure. Your provider might suggest using medical tape to hold your toes in the correct position.
- Orthotic devices: Orthotics are shoe inserts that support your feet. You might need over-the-counter orthotics or custom-made inserts. Your provider might suggest placing a spacer between your big toe and second toe, too. You may need to wear a splint to keep your big toe straight when you’re not wearing shoes.
- Pain relievers: Nonsteroidal anti-inflammatory drugs (NSAIDs) reduce pain and swelling. You might need pills you take by mouth or topical NSAIDs (creams or ointments you rub into your skin around a bunion). Don’t take NSAIDs for more than 10 days in a row without talking to your provider.
- Icing: Applying ice or cold packs to your affected toe may also help. Wrap a cold pack in a thin towel to avoid putting it directly onto your skin.
- Corticosteroids: Corticosteroids are prescription medications that reduce inflammation.
- Physical therapy: You may need to work with a physical therapist to strengthen your foot. They’ll give you exercises or stretches that may help your toes stay in better alignment.
- Surgery: Your provider may recommend bunion correction surgery if other treatments don’t relieve your symptoms or walking is extremely painful. Your provider or surgeon will tell you which type of surgery you’ll need and what to expect.
Do bunions go away on their own?
No, bunions don’t just go away and you can’t fix bunions on your own. See a healthcare provider or podiatrist if you have a bunion. They’ll diagnose it and suggest treatments to relieve your symptoms.
How can I prevent a bunion?
Since bunions are caused by a combination of several different reasons, they can be difficult to prevent. That being said, wearing well-fitting shoes may help reduce the progression of bunions. In general, follow these tips to find comfortable shoes that fit your feet properly:
- Avoid shoes with narrow, pointed tips — especially if they fit tightly on your toes
- Even if you know your size, try on a few pairs of shoes to make sure you’re getting the best fit. Labeled shoe sizes aren’t always the same between brands and styles
- Sit, stand and walk in new shoes before buying them. Make sure no movement or position hurts, pinches or pushes on your toes.
- Trying shoes on at the end of the day may give you a more accurate fit (your feet naturally swell slightly over the course of a day and are bigger later in the day than they are first thing in the morning).
- Your provider or podiatrist can recommend types or brands of shoes that’ll work well for your feet. If you have other structural foot issues like flat feet or high arch feet, ask your provider whether you need orthotics to prevent bunions.
What can I expect if I have bunions?
Most people with bunions are able to manage their symptoms with few long-term impacts to their daily routine. Your provider will work with you to find a combination of treatments to relieve your symptoms and keep your feet and toes healthy and strong.
Don’t wait to see a provider if you have bunion symptoms. The sooner you start treatment, the more likely it is you’ll be able to manage your symptoms without surgery.
People who need bunion surgery can usually resume all their usual activities in two to three months.
When should I see my healthcare provider?
Visit a healthcare provider or podiatrist as soon as you notice any of the following symptoms:
- pain in your foot or toes
- difficulty walking or moving
- a noticeable bump near the base of your big toe
- swelling in or around your toes
Bunions are a common foot issue. They happen when something pushes your big toe out of its natural alignment and toward your other toes. Eventually, a bony bump can form on the joint where your big toe meets your foot.
Bunions need treatment if they cause pain. Even if it’s a simple solution like changing the kinds of shoes you’re wearing, you still need to see a healthcare provider or podiatrist to diagnose a bunion. Your provider will suggest treatments that’ll relieve your symptoms and help you get back to the activities you love.
Can dietary supplements help give relief when you suffer from scoliosis, kyphosis or bunions?
Dietary supplements might offer some supportive benefits for managing symptoms related to scoliosis, kyphosis, or bunions, but they’re not a cure or a direct treatment for these structural conditions.
For scoliosis (sideways spinal curvature) and kyphosis (excessive forward spinal curvature), supplements like calcium and vitamin D could help maintain bone density, especially if you’re at risk for osteoporosis, which can worsen spinal issues.
Magnesium might ease muscle tension or spasms that sometimes accompany these conditions, as tight muscles can amplify discomfort.
Collagen supplements are often touted for joint and connective tissue health, but evidence is shaky on whether they significantly alter spinal alignment or pain in these cases.
Anti-inflammatory supplements like omega-3 fatty acids or curcumin might reduce general inflammation and soreness, potentially offering mild relief if pain stems from irritated tissues.
For bunions (bony bumps at the base of the big toe), the story’s similar but different. Bunions are largely mechanical—caused by joint misalignment, genetics, or footwear—so supplements won’t fix the deformity.
However, vitamin C and collagen could theoretically support cartilage and connective tissue health, possibly slowing degeneration.
Anti-inflammatory options like curcumin or ginger might help with pain or swelling in the affected area, especially if arthritis is involved.
Sadly, studies on supplements for these specific conditions are sparse. A 2018 review in Journal of Orthopaedic Research found vitamin D and calcium critical for bone health in spinal deformities, but not transformative for curvature itself.
Pain relief from anti-inflammatories is plausible but varies wildly person-to-person—placebo-controlled trials (e.g., on omega-3s for joint pain) show modest effects at best.
Real relief usually comes from physical therapy, orthotics, or, in severe cases, surgery.
Supplements might be a complementary tweak—think 10-20% symptom improvement if you’re lucky—but don’t expect them to straighten spines or shrink bunions.
Recent posts
- Better fit and fat than lazy and thin? Fit at every size, yet 'fat but healthy’ is a myth!
- Gut health and sleep: can your microbiome keep you up at night?
- Is chewing gum bad for your health? Chewing gum exposes us to microplastics and may ruin dental health
- Radiation from wearable devices, is it a reason for concern?
- Diabetes and heart disease , how they are related and what can you do about it?
- Acute versus chronic pain: what's the difference and how to get rid of it or learn to cope with it?
- How common are spinal or foot abnormalities?
- Why are fertility rates declining around the world?
- What virus have I been affected by? What is the best way to deal with a viral infection?
- On anosmia, the loss of your sense of smell and how to regain the sense of smell naturally


